The Benefits of Exercise for Parkinson’s Disease
Your family and friends are constantly encouraging you to exercise. Your doctors tell you that exercise is a vital component of Parkinson’s disease (PD) treatment. APDA programming includes exercise programs as a way for people with PD to gain control over their disease. But is exercise worth all the fuss? What does exercise actually do for someone with PD? Is there evidence that shows exercise really helps? And if it does help, are there specific types of exercise that help more than others?
I will address these fundamental questions about exercise and Parkinson’s in two parts. In today’s post, I will address why it is so important for a person with PD to exercise. My next post will address what types of exercise to consider for PD.
Exercising as we age
In general, exercise is extremely important to help people remain as healthy as possible at all points in their lives, including as they age. This holds true for the vast majority of people.
Of course, there are particular medical concerns, such as certain heart issues, that necessitate a limitation in exercise. However, there are many other disorders that may actually improve with exercise, so please be sure to talk with your doctor about all your medical conditions before embarking on any exercise plan.
Why exercise is important for people with Parkinson’s
Here are four major reasons why it is critical to exercise with Parkinson’s:
1. Epidemiological studies have demonstrated the benefits of exercise as it relates to PD risk and PD severity.
These findings are summarized in this paper and include:
- Those in midlife who routinely engage in moderate to vigorous exercise have a lower risk of developing PD than those who don’t
- Cardiovascular fitness is associated with better cognitive and motor scores in those who have PD
- Longevity in PD is associated with increased physical activity
2. Maximizing general fitness is essential to meet the challenges of Parkinson’s and other medical issues that can develop as we age
Deconditioning is a very common problem and refers to a general decrease in a person’s level of physical fitness due to a sedentary lifestyle. The deconditioned person may have trouble walking or may feel pain, stiffness, or shortness of breath with exertion. When a person is deconditioned, a vicious cycle may ensue in which the person limits his/her exercise and that limitation in exercise serves to keep the person even more unable to exercise!
Now take a deconditioned person and give them PD! It is not hard to envision how difficult that combination can be.
Therefore, starting an exercise program can build up exercise tolerance and make you more physically fit, which will put your body in a better position to face the challenges of PD.
Another important point to note is that there are a number of common medical problems that interfere with movement and can complicate a person’s Parkinson’s symptoms, and these include:
- Spinal stenosis or spinal radiculopathy – narrowing of the spaces through which the spine and the nerves that emerge from the spine travel. These conditions cause compression or irritation of the spine and/or nerves and can lead to a whole host of symptoms including lower back pain.
- Arthritis – pain, swelling and stiffness in joints throughout the body including the shoulders and knees.
- Prior strokes – Small strokes due to poor blood flow in the brain may accumulate with age and contribute to neurologic symptoms including difficulty walking
- Neuropathy – dysfunction of the nerves that travel to the feet (or hands) which can cause numbness, weakness or other sensations such as tingling or burning
- Vestibular and hearing loss – dysfunction of the nerves that feed the ear and can lead to balance difficulties
A fit body will help you overcome the challenges of all these conditions. So don’t use these as excuses not to exercise. There are many different types of exercise and many modifications that can be made so that people can get the benefits of exercise despite other issues they may have.
The process of becoming more physically fit takes time and typically requires input from a physical therapist and/or a fitness professional – preferably one who understands PD. APDA has developed a specialized training program for fitness professionals to help them understand what PD is and how to best work with a person who has PD.
3. Exercise has been shown to improve specific symptoms that commonly affect people with Parkinson’s
PD is associated with a long list of both motor and non-motor symptoms, many of which can be improved with exercise. In this paper, the authors review the evidence of the health benefits of exercise that can be particularly impactful on people with PD including:
- Improved cognitive function
- Improved depression
- Improved sleep
- Decreased constipation
- Decreased fatigue
- Stop or slow osteoporosis – exercise improves bone strength, which means less of a chance that a PD-related fall will lead to a fracture
- Improved motor performance – exercise can improve strength, balance, posture and gait, among other measures of motor functioning
- Improved drug efficacy – exercise may increase levodopa absorption making medications more impactful
4. Exercise can be neuroprotective in Parkinson’s
The above reasons are certainly enough to champion exercise for people with PD, but there is a fourth, potentially even more critical reason that exercise is vital in PD – its potential to promote neuroprotection.
Neuroprotection refers to the ability of a treatment to preserve the neurons in the brain from deteriorating – and that is what is necessary to slow down or halt the progression of diseases like PD in which nerves degenerate and die. Although there are many clinical trials of potential medications that may offer neuroprotection, as of now there is no FDA approved medication that can do this. Therefore, our best bet is exercise.
This review paper summarizes the data on how exercise in people with PD reinforces the brain’s ability to form and reorganize neural connections and repair damaged ones. Evidence exists that exercise can contribute to neuroprotection in the following ways:
Increasing dopamine signaling:
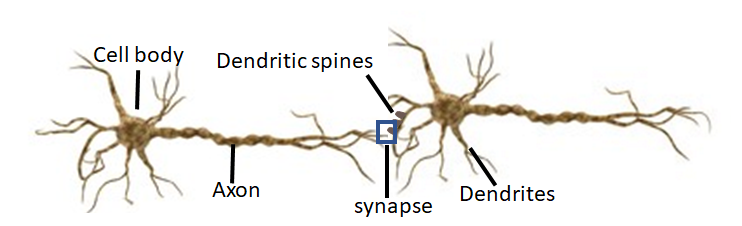
It will help here to have a basic understanding of what dopamine signaling is. These two figures below will help. The first figure shows two neurons which are in communication with each other. The axon of the first neuron lies very close to the dendrites of the second neuron. The dendrites are covered with small protrusions called dendritic spines which increase the number of connections one neuron can make with other neurons. The space between two neurons is called a synapse, which is demarcated by the blue box. The second picture is a close-up of a synapse.
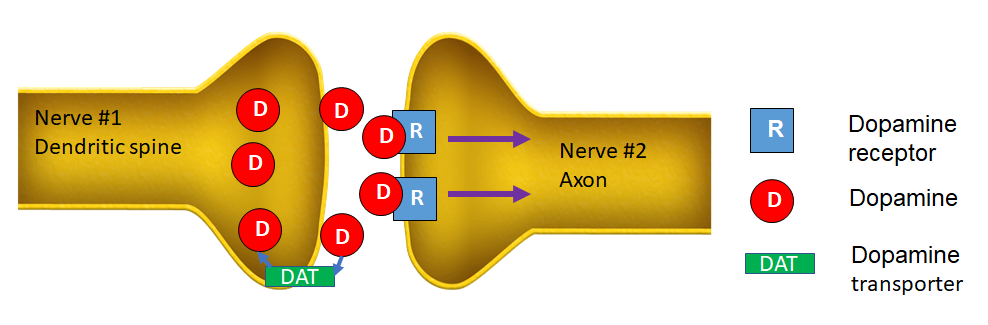
In the second figure, a message travels down the first neuron and reaches the end of the axon. Dopamine is released from the first neuron into the synapse. Dopamine receptors on the second neuron interact with the dopamine and allow for continuation of the signal down the second neuron. On the surface of the first neuron is a molecule called the dopamine transporter. Its job is to retrieve the dopamine from the synapse after the communication is over.
There is evidence from animal studies that exercise may contribute to an increase in dopamine signaling in a variety of ways:
- Enhanced release of dopamine into the synapse
- Decreased clearance of dopamine from the synapse. This is accomplished by reducing the expression of the dopamine transporter molecule whose role it is to remove dopamine from the synapse
- Increased dopamine receptor density which allows for the available dopamine to interact with its neighboring neurons more efficiently
- Increased dendritic spine formation or reversal of dendritic spine loss which creates more space for dopamine signaling to take place
Improving overall brain health through:
- Increased nerve growth factors which encourage nerves to sprout new connections and maintain their health
- Increased blood flow by increasing blood vessel production in the brain. This improves the availability of oxygen and glucose to the brain, as well as other signaling molecules including nerve growth factors
- Promotion of beneficial changes to the brain immune system
- Increased neurogenesis or production of new nerve cells. Certain areas of the adult brain maintain the capacity to produce new neurons. Exercise may increase this capability
Exercise can improve your fitness level, making your body more able to combat the challenges of PD and other disorders of aging. It can help improve particular motor and non-motor symptoms of PD. Finally, it may work to keep neurons alive, healthy, and functioning properly in the brain, staving off PD’s effects.
To help you get started and to get the most out of your exercise, APDA has developed a variety of resources:
- Be Active & Beyond (English) – A guide to specific exercises for people with PD that you can do at home, with pictures that you can follow. For all fitness and mobility levels. (Also available in Spanish.)
- Let’s Keep Moving With APDA – This webinar series is hosted by professional physical therapists and offers tips, research, and news on staying active and exercising.
- APDA supports the APDA National Rehabilitation Resource Center for Parkinson’s Disease located at Boston University Sargent College Center for Neurorehabilitation. The Center can be reached via a helpline (1-888-606-1688) or email (rehab@bu.edu) and is available to answer your exercise or physical therapy related questions.
Tune in next week when I will address what types of exercise to consider for your exercise regimen.
Tips and takeaways
- Exercise is a vital component of Parkinson’s treatment
- Exercise can improve your fitness level, making your body more able to combat the challenges of PD and other medical conditions
- There is evidence that exercise can improve particular motor and non-motor symptoms of PD such as impaired balance, gait disorders, depression and cognition
- There is evidence that exercise may improve brain functioning in a number of ways
- APDA has a variety of resources to help you exercise at your best, no matter what your current fitness level is

